46 year old with chest pain develops a wide complex rhythm -- see many examples
Dr. Smith's ECG Blog
AUGUST 9, 2024
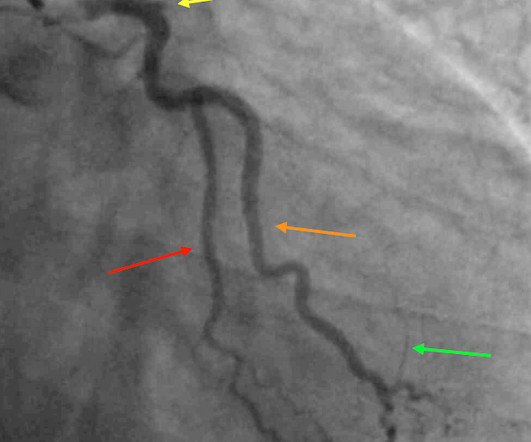
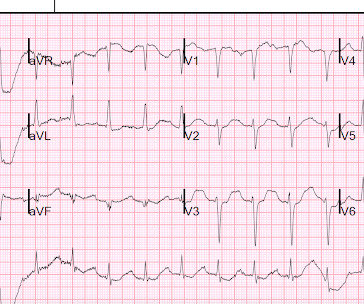
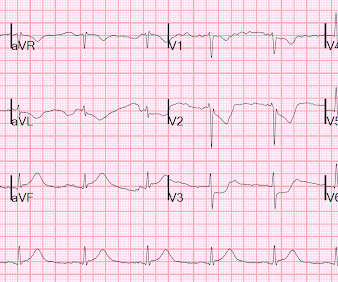
These diagnoses were not found in his medical records nor even a baseline ECG. He had no previously documented medical problems except polysubstance use. An ECG was obtained shortly after arrival: What do you think? There is no evidence of WPW on this ECG, but it is diagnostic for OMI. What are we seeing here?










Let's personalize your content